
Erasmus+
“This project has been funded with support from the European Commission. This publication reflects the views only of the author, and the Commission cannot be held responsible for any use which may be made of the information contained therein”
Wrestler’s knee common Injuries
Upon completion of this module the reader will be able to:
- Understand basic anatomy and functional anatomy for the lower limbs complex.
- Understand the knee Injury epidemiology
- Understand the mechanisms for the ankle and knee injuries.
- Determine common risk factors that can lead to the ankle and knee injuries.
- Incorporate exercises in order apply a prevention strategy for the ankle and knee injuries Meniscus injuries.
- Review the «Anatomy and Functional of the knee joint» topic and the «Injury prevention strategies». Read the description of the “Lower limb Prevention strategies” and the corresponding presentation and then follow the proposed videos for some ideas of “Lower limb prevention exercises”. End the session with the “Bibliography and the additional learning materials” and assess your understanding with the “Lower limb injuries”
The soft tissue structure in the knee includes 2 menisci, the MM (located on the inside of the knee) and LM (located on the outside of the knee). These crescent-shaped pads of fibrocartilage rest on the tibial condyles and form a concave surface for the femoral condyles to rest on.
These cover approximately 2/3 of the tibia surface and are thicker on the outside and thinner on the inside appearing triangular in cross section. They fill the space between the leg bones and cushion the femur so it doesn’t slide off or rub against the tibia. The menisci play a very important role in the proper working of the knee. Essentially, they serve as cushions to decrease the stress caused by weight bearing and forces on the knees.
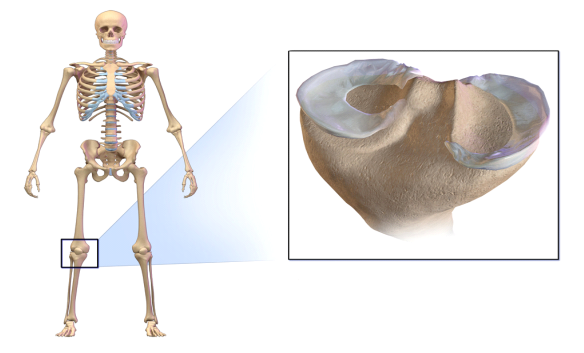
By Andrewmeyerson – Own work, CC BY-SA 4.0, https://commons.wikimedia.org/w/index.php?curid=49411618
Figure: An illustration of knee joint and the menisci. The menisci are “thin discs” that lie between the thigh (upper leg) and the tibia (lower leg)
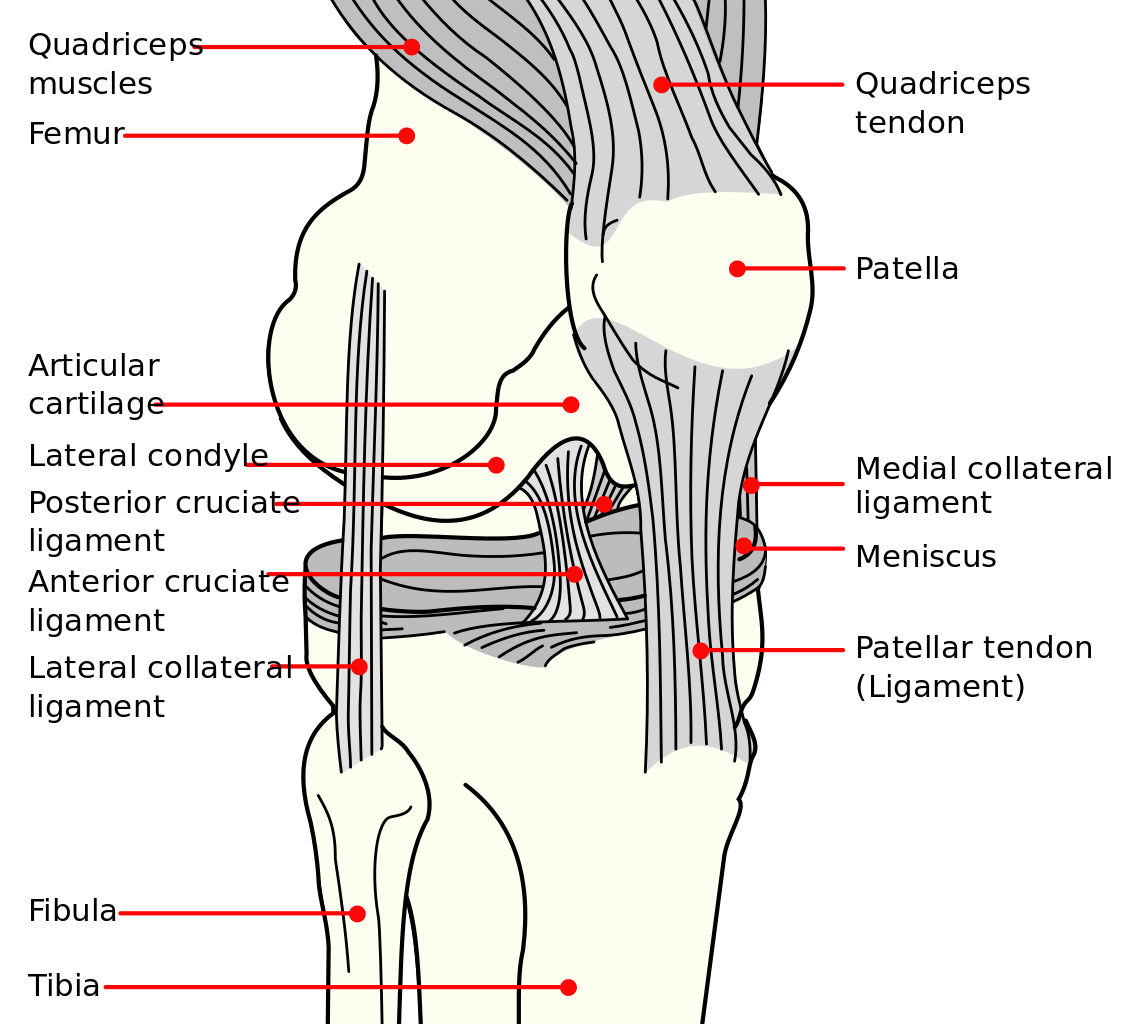
They work like shock absorbers, supporting the load by compressing and spreading the weight evenly within the knee. The menisci assist with the proper movement (arthrokinematic) of the femur and tibia during flexion and extension. They help stabilize the knees when in motion, reduce friction within the joint, and lubricate and protect the articular cartilage surrounding the tips of the bones from damage due to wear and tear.
Knee
The lower extremity is classically the most commonly injured area in wrestling with more number of injuries occurring at the knee followed by the ankle (Strauss & Lanese, 1982; Pasque & Hewett, 2000). These injuries are usually season ending and often require surgical intervention.
Knee injuries are more common in college wrestlers, not only in frequency, but also in severity. Knee injuries are the most common injury responsible for missing 3 weeks or more of college wrestling and the most common site of injury requiring surgery (Yard et al., 2008).
In Agarwal & Mann (2016) study more number of knee injuries occurred in attack position. This can possibly be attributed to poor technique. More number of knee injuries i.e. 93.33%, were sustained in competitions while only 4.49% injuries occurred during practice in Agarwal & Mann (2016) study (incidence density ratio = 20.7). In Agarwal & Mann (2016) study 60.56% knee injuries occurred in the age group of 20 – 24 years, while 29.57% injuries were seen in the age group of 15 – 19 years. Out of total knee injuries, 61.97% injuries occurred in wrestlers practicing for 5 – 10 years, while 35.21% occurred in wrestlers practicing for 0 – 5 years. Use of legs in FS and hands and arms in GR as per rules possibly makes these wrestlers more vulnerable to lower and upper extremity injuries, respectively.
In Agarwal & Mann (2016) study 83.09% injuries occurred in FS wrestlers while 16.90% occurred in GR wrestlers. The proportion of injuries i.e. total knee injuries in wrestlers practicing FS wrestling was also more (IPR = 1.39). A study by Wroble et al. (1986) revealed that there were 11.5 knee injuries per 100 wrestlers per year requiring a week or greater time loss. Pasque & Hewett, (2000) found that the mean total time lost from injury was 5 days (range, 1 – 39days). There were 18.11 knee injuries per 100 wrestlers per year requiring a week or greater time loss in our study.
In prospective studies, knee injuries have ranged from 7.6 to 44% of all wrestling injuries (Strauss & Lanese, 1982; Hewett et al., 2005). In the only study with the percentage of knee injuries below 10%, Lorish et al. (1992) described injuries in tournaments to wrestlers aged 6 – 16 years. The knee injuries, in Agarwal & Mann (2016) study also were quite high comprising 37.7% of all injuries reported. These injuries tend to be severe. Over an 11 year period in NCAA wrestling, 65% of injuries requiring surgery involved the knee. In the same study, 21% of injuries leading to greater than one week absence from competition involved the knee (Jarret et al., 1998). Barroso et al. (2011) in their study found that the highest number of lesions involved the knee (25.5%), followed by the shoulder (20%) (Barroso et al., 2011). However, more number of injuries occurred to the shoulder (24%) followed by the knee (17%) in a study by Pasque & Hewett, (2000).
According to Wroble et al. (1986) wrestlers with previous knee injuries were at high risk for re-injury. Kordi et al. (2012) reported that 77% of all injuries were acute ones (new injuries), 10% of injuries were recurrent, 2% of injuries were unresolved injury from the preceding year and 1% of them were due to a recent worsening of an unresolved injury. In Agarwal & Mann (2016) study 71.83% of the knee injuries were new injuries while, 28.16% were recurrent. The most common knee injuries are sprains, which constitute 30 – 65% of all knee injuries.
Prepatellar bursitis is a very common type of knee injury, and is fairly unique to wrestling (Strauss & Lanese, 1982; Mysnyk et al., 1986). Mysnyk et al. (1986) documented 28 cases of prepatellar bursitis, representing 21% of all knee injuries.
Meniscus
The soft tissue structure in the knee includes 2 menisci, the MM (located on the inside of the knee) and LM (located on the outside of the knee). These crescent-shaped pads of fibrocartilage rest on the tibial condyles and form a concave surface for the femoral condyles to rest on. These cover approximately 2/3 of the tibia surface and are thicker on the outside and thinner on the inside appearing triangular in cross section. They fill the space between the leg bones and cushion the femur so it doesn’t slide off or rub against the tibia. The menisci play a very important role in the proper working of the knee. Essentially, they serve as cushions to decrease the stress caused by weight bearing and forces on the knees. They work like shock absorbers, supporting the load by compressing and spreading the weight evenly within the knee. The menisci assist with the proper movement (arthrokinematic) of the femur and tibia during flexion and extension. They help stabilize the knees when in motion, reduce friction within the joint, and lubricate and protect the articular cartilage surrounding the tips of the bones from damage due to wear and tear.
Meniscal injuries are also common, with a relatively high proportion of lateral to medial meniscus tears (Hewett et al., 2005). Lateral meniscus injuries represented 46% of the total number of meniscal injuries in a study and there were 45% lateral versus medial meniscectomy in a study on 56 meniscectomies in wrestlers (Strauss & Lanese, 1982; Baker et al., 1985). Lateral meniscus injuries were 58.3% of all meniscal injuries in Agarwal & Mann (2016) study.
ACL
The ACL originates from the medial and anterior aspect of the tibial plateau and runs superiorly, laterally, and posteriorly toward its insertion on the lateral femoral condyle. The ACL is composed of the anteriomedial and posteriolateral bundles. Together, these bundles provide approximately 85% of total restraining force of anterior translation. It also prevents excessive tibial medial and lateral rotation, as well as varus and valgus stresses. To a lesser degree, the ACL checks extension and hyperextension. Together with the posterior cruciate ligament (PCL), the ACL guides the instantaneous center of rotation of the knee, therefore controlling joint kinematics.
Anterior cruciate ligament (ACL) ruptures are among the most commonly studied injuries in orthopaedic research. The incidence of ACL ruptures is estimated to range from 30 to 78 per 100,000 person-years. After ACL reconstruction, 61% to 89% of athletes successfully return to sports, typically at 8 to 18 months after reconstruction, depending on the level of play.
Anterior cruciate ligament tears were noted in 14 of 256 knee injuries in one study (Strauss & Lanese, 1982). Similarly, three of the 64 knee injuries were ACL tears in a study by Wroble et al. (1986). In Agarwal & Mann (2016) study 8/77 injuries were ACL tears.
MCL
The medial collateral ligament (MCL) of the knee is the major stabilizer against valgus force and is frequently placed under great stress in the sport of wrestling (Kiningham & Monseau, 2015).
MCL injuries are relatively common in young athletes. Most injuries occur with direct contact, placing a valgus force on the knee, or from cutting maneuvers with the foot planted, creating a valgus moment in the knee. The addition of a rotational force may injure the posterior oblique ligament as well as the MCL (Indelicato, 1995). The 3-layer concept of the anatomy of the medial knee described by Warren and Marshall (1979) notes that after the superficial sartorial fascial layer, the middle layer contains the superficial MCL and posterior oblique ligament, and the deep layer contains the true capsule of the knee joint and the deep MCL.
Usually, MCL injuries are graded based on the American Medical Association’s classification according to the medial knee opening with valgus stress placed with the knee in 30° of flexion. Grade 1 opens <5 mm, grade 2 opens between 5 and 10 mm, and grade 3 opens >10 mm (American Medical Association, 1966). The vast majority of MCL injuries are treated nonoperatively with emphasis on early rehabilitation, range of motion exercises, and weightbearing when pain free (Miyamoto, et al., 2009). Despite the lack of surgical management, these common injuries can cause significant lost time to return to sport or activity.
The overall IR of MCL injuries in a young athletic cohort was 7.27 per 1000 person-years. Male intercollegiate athletes were over 2.6 times more likely to sustain an MCL injury than female intercollegiate athletes (Roach et al., 2014). The intercollegiate sports of wrestling, judo, hockey, and women’s rugby had the highest IRs of MCL injuries. There were 73% grade 1 MCL injuries, while 27% were grade 2 or 3. The average amount of time lost per injury was 23.2 days, with greater time lost with higher grade sprains than grade 1 sprains (Roach, et al., 2014).
Knee’s injuries prevention exercises for wrestlers
Phase I : Muscular conditioning to restore dysfunctional movement patterns that can impede performance
Phase II: Functional exercise – Building efficient movement pattern
Bibliography and the additional learning materials
- First try to increase your joint flexibility using stretches
- Strengthen you muscles, especially the quadriceps
- Perform balance exercises
- Try to improve your technique in landings and changes in direction
- Always exercise in a pain-free range of motion. Exercises or parts of exercise that lead to pain should be avoided.
Agarwal S. & Mann E. (2016). Knee Injuries in Wrestlers: A Prospective Study from the Indian Subcontinent. Asian J Sports Med. 2016; 7(4): doi: 10.5812/asjsm.35000.
Agel, J., Ranson, J., Dick, R., Opplinger, R., & Marshal S. (2007). Descriptive epidemiology of collegiate men’s wrestling injuries: National Collegiate Athletic Association Injury Surveillance System, 1988–89 through 2003–2004. Journal of Athletic Training, 42(2), 303–310.
Akbarnejad A, Sayyah M. (2012) Frequency of sports trauma in elite national level greco-roman wrestling competitions. Arch Trauma Res. 2012;1(2):51–3.
American Medical Association, Committee on the Medical Aspects of Sports. Standard Nomenclature of Athletic Injuries. Chicago: American Medical Association; 1966.
Armstrong A. (2015). Simple elbow dislocation. Hand Clin. 2015;31(4): 521-531.
Baker BE, Peckham AC, Pupparo F, Sanborn JC. (1985) Review of meniscal injury and associated sports. Am J Sports Med. 1985;13(1):1–4.
Barroso BG, Silva JMA, Garcia AC, Ramos NCO, Martinelli MO, Resende VR, et al. (2011) Musculoskeletal injuries in wrestling athletes. Acta Ortop Bras. 2011;19(2):98–101.
Boden BP, Lin W, Young M, Mueller FO. (2002) Catastrophic injuries in wrestlers. Am J Sports Med. 2002;30(6):791-795.
Borowski LA, Yard EE, Fields SK, Comstock RD. (2008) The epidemiology of US high school basketball injuries, 2005Y2007. Am. J. Sports Med. 2008; 36(12): 2328-35.
Brindle, T. J., & Cohen, M. (1998). Scapular avulsion fracture of a high school wrestler. Journal of Orthopaedic & Sports Physical Therapy, 27(6), 444–447.
Centers for Disease Control and Prevention. (2006). Sports related injuries among high school athletes—United States, 2005–2006 school year. Morbidity and Mortality Weekly Report, 296(22).
Chaabene H, Negra Y, Bougezzi R, et al. (2017) Physical and physiological attributes of wrestlers: an update. J Strength Cond Res. 2017;31 (5):1411–1442.
Garrick J: Ankle injuries: Frequency and mechanism of injury. Athletic Training 1975;10:109–111.
Gonell, A.C.; Romero, J.A.P.; Soler, L.M. (2015). Relationship between the Y Balance Test Scores and Soft Tissue Injury Incidence in a Soccer Team. Int. Sports Phys. Ther. 2015, 10, 955–966.
Goodman AD, Twomey-Kozak J, DeFroda SF, Owens BD. (2018) Epidemiology of shoulder and elbow injuries in National Collegiate Athletic Association wrestlers, 2009–2010 through 2013–2014. The Physician and Sportsmedicine. 2018;46(3):361–366.
Halloran L. (2008). Wrestling Injuries. Orthopaedic Nursing (2008) 27(3), 189-192
Hassebrock J.D., Patel, K.A., Makovicka J.L., Chung A.S., Tummala S.V., Hydrick T.C., Ginn J.E., Hartigan D.E., Chhabra A. (2019). The Orthopaedic Journal of Sports Medicine, (2019), 7(8), 1-10.
Haugegaard M, Rasmussen S, Johannsen P. (1993). Avulsion fracture of the medial humerus epicondyle in young wrestlers. Scand J Med Sci Sports 1993;3:178–181.
Hermans JJ, Beumer A, de Jong TA, Kleinrensink GJ. (2010) Anatomy of the distal tibiofibular syndesmosis in adults: a pictorial essay with a multimodality approach. J Anat. 2010;217(6):633-645.
Hetrel J. (2002). Functional Anatomy, Pathomechanics, and Pathophysiology of Lateral Ankle Instability. J Athl Train, 2002 37(4): 364–375.
Hewett TE, Pasque C, Heyl R, Wroble R. (2005) Wrestling injuries. Med Sport Sci. 2005;48:152–78.
Hunt KJ, Phisitkul P, Pirolo J, Amendola A. (2015) High ankle sprains and syndesmotic injuries in athletes. J Am Acad Orthop Surg. 2015;23(11): 661-673.
Indelicato PA. (1995). Isolated medial collateral ligament injuries in the knee. J Am Acad Orthop Surg. 1995;3:9-14.
Jarret GJ, Orwin JF, Dick RW. (1998) Injuries in collegiate wrestling. Am J Sports Med. 1998;26(5):674–80.
Jlid MC, Maffulli N, Elloumi M, Moalla W, Paillard T. (2013) Rapid weight loss alters muscular performance and perceived exertion as well as postural control in elite wrestlers. Journal of Sports Medicine and Physical Fitness. 2013;53(6):620–627.
Kabak, B.; Karanfilci, M.; Karakuyu, N.A. (2017) Comparison of Sports Injuries in Judo and Wrestling Sports. J. Sports Perform. Res. 2017, 8, 107–122.
Kaplan LD, Jost PW, Honkamp N, Norwig J, West R, Bradley JP. (2011) Incidence and variance of foot and ankle injuries in elite college football players. Am J Orthop (Belle Mead NJ). 2011;40(1):40-44.
Karbach LE, Elfar J. (2017). Elbow instability: anatomy, biomechanics, diagnostic maneuvers, and testing. J Hand Surg Am. 2017;42(2):118-126.
Kiningham R., Monseau A. (2015). Caring for Wrestlers. Current Sports Medicine Reports, 2015, 14(5),404-412
Kleeman LT, et al. (2015) .Cervical Spine Injuries In Sports. The Duke Orthopaedic Journal 2015; 5(1): 58-62
Kordi R, Ziaee V, Rostami M, Wallace WA. (2012). Sports injuries and health problems among wrestlers in Tehran. J Pak Med Assoc. 2012;62(3):204–8.
Kordi R., Heidarpour B., Shafiei M., Rostami M., Mansournia M.A. (2012) Incidence, Nature, and Causes of Fractures and Dislocations in Olympic Styles of Wrestling in Iran: A 1-Year Prospective Study. Sports Health, 4(3), 217-221.
Lievers WB, Adamic PF. (2015) Incidence and severity of foot and ankle injuries in men’s collegiate American football. Orthop J Sports Med. 2015; 3(5):2325967115581593.
Lorish TR, Rizzo TD, Ilstrup DM, Scott SG. (1992) Injuries in adolescent and preadolescent boys at two large wrestling tournaments. Am J Sports Med. 1992;20(2):199–202.
Maffulli N. (1992). Making weight: a case study of two elite wrestlers. British Journal of Sports Medicine. 1992;26(2):107–110.
Markolf KL, Jackson SR, McAllister DR. (2013) Syndesmosis fixation using dual 3.5 mmand 4.5 mm screws with tricortical and quadricortical purchase: a biomechanical study. Foot Ankle Int. 2013;34(5):734-739.
Mauntel T.C., Erik A. Wikstrom E.A., Roos K.G., Djoko A., Dompier T.P., Kerr Z.Y. (2017). The Epidemiology of High Ankle Sprains in National Collegiate Athletic Association Sports The American Journal of Sports Medicine, 45(9), 2156-2163.
Miller, L.E.; Pierson, L.M.; Nickols-Richardson, S.M.; Wootten, D.F.; Selmon, S.E.; Ramp, W.K.; Herbert, W.G. (2006). Knee Extensor And Flexor Torque Development With Concentric And Eccentric Isokinetic Training. Res. Q. Exerc. Sport 2006, 77, 58–63.
Miyamoto RG, Bosco JA, Sherman OH. (2009). Treatment of medial collateral ligament injuries. J Am Acad Orthop Surg. 2009;17:152-161.
Mudgal, C., & Waters, P. (1998). Isolated fracture subluxation of the second sternocostal synchodrosis: A case report. The American Journal of Sports Medicine, 26(5), 729–730.
Myers RJ, Linakis SW, Mello MJ, Linakis JG. (2010) Competitive Wrestlingrelated Injuries in School Aged Athletes in U.S. Emergency Departments. West J Emerg Med. 2010;11(5):442–9.
Mysnyk MC, Wroble RR, Foster DT, Albright JP. (1986) Prepatellar bursitis in wrestlers. Am J Sports Med. 1986;14(1):46–54.
Park K.J, Lee J.H, Kim H.C. (2019). Injuries in male and female elite Korean wrestling athletes: a 10-year epidemiological study. Br J Sports Med. 2019 Apr;53(7):430-435.
Pasque CB, Hewett TE. (2000) A prospective study of high school wrestling injuries. Am J Sports Med. 2000; 28(4):509–15.
Pereira BP. (2013). Revisiting the anatomy and biomechanics of the anconeus muscle and its role in elbow stability. Ann Anat. 2013;195(4):365-370.
Powell JW, Barber-Foss KD. (1999) Injury patterns in selected high school sports: a review of the 1995-1997 seasons. J Athl Train. 1999;34(3):277–84.
Rahman RK, Levine WN, Ahmad CS. (2008). Elbow medial collateral ligament injuries. Curr Rev Musculoskelet Med. 2008;1(3-4):197-204.
Reichel LM, Milam GS, Sitton SE, Curry MC, Mehlhoff TL. (2013) Elbow lateral collateral ligament injuries. J Hand Surg Am. 2013;38(1):184-201.
Rineer CA, Ruch DS. (2009). Elbow tendinopathy and tendon ruptures: epicondylitis, biceps and triceps ruptures. J Hand Surg Am. 2009;34(3):566-576.
Roach C.J., Chad A. Haley C.A., Cameron K.L., Pallis M., Svoboda S.J. Owens B.D. (2014). The Epidemiology of Medial Collateral Ligament Sprains in Young Athletes. The American Journal of Sports Medicine, 42, 5, 1103-1109.
Sakali, F.M.H. (2008). Sporda Sporcuların Yaralanması Ve Risk Faktörleri. Fırat Sa˘glık Hizmetleri Dergisi 2008, 3, 143–152.
Shadgan B, Feldman BJ, Jafari S. (2010) Wrestling injuries during the 2008 Beijing Olympic Games. Am J Sports Med. 2010;38(9):1870-6.
Shadgan B, Molnar S, Sikmic S, Chahi A. (2017) Wrestling injuries during the 2016 Rio Olympic Games. British Journal of Sports Medicine. 2017;51:387.
Snook GA. (1980). A survey of wrestling injuries. Am J Sports Med. 1980;8(6):450-453.
Snook GA. (1982) Injuries in intercollegiate wrestling. A 5-year study. Am J Sports Med. 1982;10(3):142–4.
Strauss RH, Lanese RR. (1982). Injuries among wrestlers in school and college tournaments. JAMA. 1982;248(16):2016–9.
Thomas RE, Zamanpour K. (2018) Injuries in wrestling: systematic review. The Physician and Sportsmedicine. 2018;46(2):168–196.
Warren LF, Marshall JL. (1979). The supporting structures and layers on the medial side of the knee: an anatomical analysis. J Bone Joint Surg Am. 1979;61:56-62.
Waterman BR, Belmont PJ Jr, Cameron KL, Svoboda SJ, Alitz CJ, Owens BD. (2011). Risk factors for syndesmotic and medial ankle sprain: role of sex, sport, and level of competition. Am J Sports Med. 2011;39(5):992-998.
Williams BT, Ahrberg AB, Goldsmith MT, et al. (2015) Ankle syndesmosis: a qualitative and quantitative anatomic analysis. Am J Sports Med. 2015;43(1):88-97.
Wroble RR, Mysnyk MC, Foster DT, Albright JP. (1986). Patterns of knee injuries in wrestling: a six year study. Am J Sports Med. 1986;14(1):55–66.
Yard EE, Collins CL, Dick RW, Comstock RD. (2008). An epidemiologic comparison of high school and college wrestling injuries. Am. J. Sports Med. 2008; 36(1):57-64.
Yard EE, Comstock RD. (2008). A comparison of pediatric freestyle and Greco- Roman wrestling injuries sustained during a 2006 US national tournament. Scand J Med Sci Sports. 2008;18(4):491–7.
Yard, E. E. (2008). An epidemiologic comparison of high school and college wrestling injuries. The American Journal of Sports Medicine, 36(1), 57–64.
[ays_quiz id=’33’]
Erasmus+
“This project has been funded with support from the European Commission. This publication reflects the views only of the author, and the Commission cannot be held responsible for any use which may be made of the information contained therein.”
